Medicaid is the largest healthcare insurer in the U.S. Accessing health insurance through Medicaid reduces financial stress and increases access to mental health care among low-income Americans.
In 1981, Congress established the Section 1915(c) waiver program, which provides many Medicaid recipients with home-based alternatives to institutional-level care like nursing homes. These Home and Community Based Services, (HCBS), help many Medicaid recipients who would otherwise need inpatient care remain in the community. Since these programs were established, Medicaid’s long-term care spending has shifted significantly from institutional care to home-based care. The programs have improved end-of-life experiences for economically vulnerable older adults and quality of life for patients with intellectual and developmental disabilities.
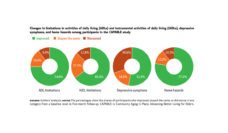
Before the pandemic, health systems struggled to support high-need patients, but these struggles intensified due to COVID-19 distancing precautions and staffing shortages. As a response to the emergency, many state Medicaid programs increased options for patients to self-direct their home care. A group of researchers led by Joseph Caldwell analyzed 36 Medicaid recipients’ experiences accessing this new level of autonomy in their care.
Medicaid recipients who self-directed their care during COVID reported many benefits from the added flexibility. Without self-direction, patients receive care through an agency that might change caregivers from week to week and rely on staffing availability. Patients’ increased autonomy in hiring or firing helped them choose caregivers they knew and trusted to provide daily care. For example, a patient could hire a family member from inside their COVID bubble instead of enduring a changing cast of caregivers in the home. The ability to hire family members seemed particularly useful for individuals from racial and ethnic minority groups.
With more funding available for these programs, now is the time for states to implement permanent changes to better meet the needs of Medicaid recipients.
Most expansions of self-direction in HCBS programs were part of the COVID public health emergency and were designed to be temporary. The American Rescue Plan, enacted in January 2021, provided $12.7 billion in enhanced federal funding for HCBS. States have until March 2024 to spend the new funds. Additionally, the Biden Administration has proposed providing significant federal investment in HCBS through the American Jobs Plan.
Federal programs incentivizing states to redirect spending from institutional settings to home and community settings have shown positive impacts on Medicaid care planning. States could use the funds to build infrastructure that supports self-directed home and community services. A 2021 survey of Medicaid HCBS programs showed that HCBS programs should allocate more funding to workforce recruitment, provider payment rate increases, programs to facilitate vaccine access, and outcomes evaluation.
Even before the advent of COVID, most people with intensive healthcare needs preferred to remain in the community. The COVID emergency presented new challenges for patients receiving care at home, but some state Medicaid solutions improved accessibility for patients beyond COVID. Better telehealth access and increased staffing control were welcome changes for many participants. Twenty-six states have proposed putting some of their additional funds toward better care coordination for program beneficiaries, as well as addressing much-needed housing assistance.
With more funding available for these programs, now is the time for states to implement permanent changes to better meet the needs of Medicaid recipients. Caldwell and his team recommend long-term changes to increase self-direction in Medicaid HCBS programs, and using additional revenues for HCBS’s based on community stakeholder input.
Photo via Getty Images