As people age, day-to-day activities like dressing, bathing, walking up and down the stairs, and managing medications tend to become more difficult and, as a result, more dangerous. Around $219 billion per year is spent on long-term care for those for whom the ability to function independently is impaired.
One alternative to costly assisted living programs or nursing homes is an innovation known as the Community Aging in Place, Advancing Better Living for Elders (CAPABLE) program. CAPABLE aims to help elderly folks with physical disabilities overcome individual or environmental limitations so as to “age in place,” which the U.S. Centers for Disease Control defines as “the ability to live in one’s own home and community safely, independently, and comfortably, regardless of age, income, or ability level.”
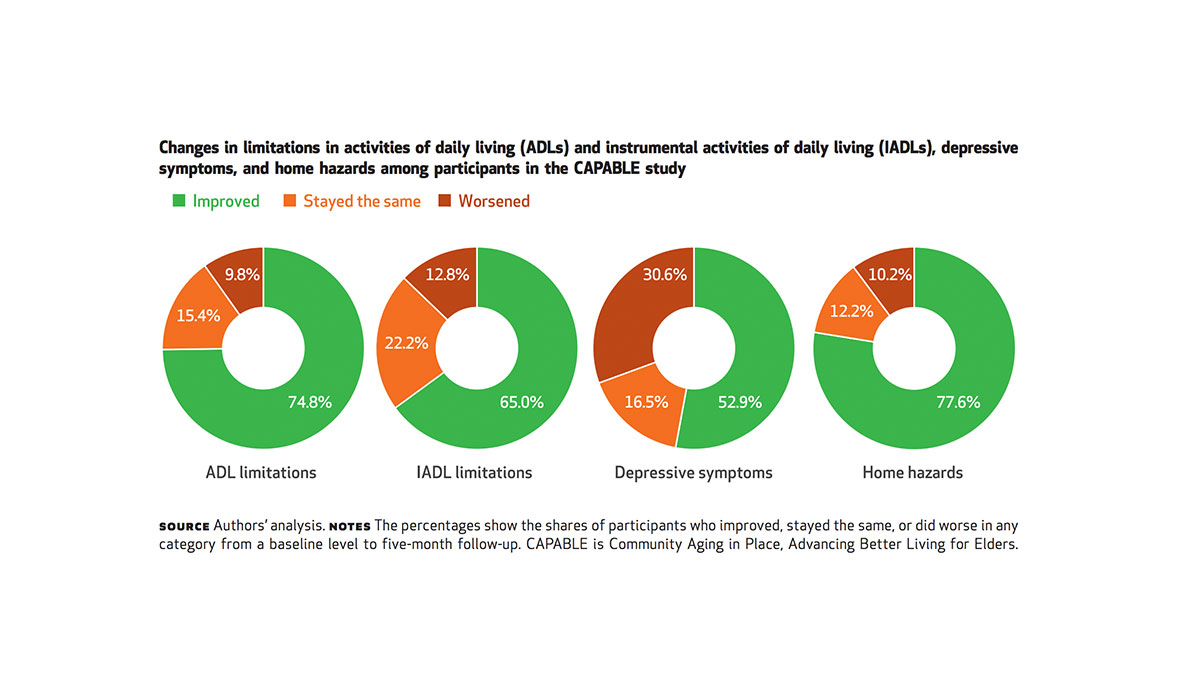
At the end of CAPABLE’s 5-month program, 75% of participants were better able to carry out their “activities of daily living” (ADLs).
As Sarah L. Szanton and her research team found in their study of the effectiveness of the CAPABLE program, health outcomes can improve through straightforward upgrades in older, low-income folks’ everyday lives. In this home-based care model, participants would set goals with a registered nurse and an occupational therapist related to independent functioning. A handyman would also work to install assistive devices, complete home repairs, and increase the safety and overall navigability of homes.
At the end of CAPABLE’s 5-month program, 75% of participants were better able to carry out their “activities of daily living” (ADLs). On average, participants were able to reduce their difficulties with ADLs from 4 to 2, which also appeared to reduce symptoms of depression and existence of home hazards.
Based on these results, the broad use of home-based modifications for those with physical disabilities can save older folks and their families money on housing and health care alongside much-needed improvements in quality of life and mental health.
Databyte via Sarah L. Szanton et al., Home-Based Care Program Reduces Disability And Promotes Aging In Place. Health Affairs.