Eating disorders are hard to understand and even harder to treat, even with the best resources. Unfortunately, few resources are available and some of the most pernicious and lethal mental health diagnoses – anorexia nervosa and bulimia nervosa – are often excluded from insurance coverage altogether.
This lack of insurance coverage exists despite decades of gradually improving mental health parity legislation. Plans available through the Affordable Care Act’s (ACA) marketplace include mental health coverage parity as established by the Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA) which requires parity in mental and physical health coverage in those plans which offer mental health coverage.
The critical loophole in the ACA’s and MHPAEA’s mental health parity requirements is the state-by-state determination of what qualifies as mental illness, how mental illnesses can be diagnosed, and what qualifies as necessary treatment. It’s this state-level variation which frequently excludes eating disorders from the conditions requiring coverage under existing mental health parity laws.
Advocates of all stripes are pushing for increased access insurance coverage for eating disorder treatment. This coalition includes individuals and families impacted by eating disorders, resource and engagement organizations, and professional groups such as the AMA. Their efforts range from development and promotion of national policy to professional commitments to parity in treatment to dissemination of language and strategies for justifying treatment needs to insurance companies.
The mortality rate of anorexia nervosa is 10%, and doubles to 20% when suicide by patients with anorexia is included, making it the most lethal mental illness in the United States.
This push is absolutely critical because eating disorder treatment saves lives . The mortality rate of anorexia nervosa is 10%, and doubles to 20% when suicide by patients with anorexia is included, making it the most lethal mental illness in the United States. Facing such odds, families will do everything they can to help their ill loved ones, but available treatments are unpredictable in efficacy, limited in accessibility, and extremely expensive.
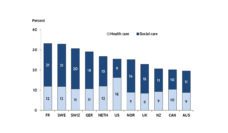
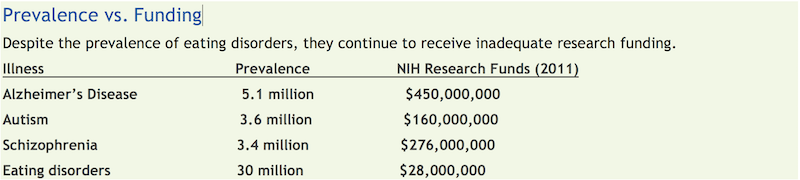
Eating disorder research is a newer field, and the complex mixture of chemical, cognitive, emotional, and environmental factors which appear to instigate and then maintain these illnesses complicate the practice recommendations which arise from this research. Further limiting the scope and utility of current research is the comparatively limited funding afforded this crippling group of disorders. As illustrated below, research funding per affected person is more than $80 for Alzheimer’s and Schizophrenia, more than $40 for Autism, but less than $1 for all eating disorders.
Despite the grave consequences of eating disorders and the developing nature of research and treatment knowledge to address them, there are reasons for hope and action. Eating disorder research is ongoing and is continually unearthing new details about the etiology of the illnesses and generating new treatment programs, which are working. These promising steps suggest increased research funding, expanded insurance coverage of treatment, and universal recognition of eating disorders as serious mental illnesses can further the important progress being made to support recovery for the millions of people fighting them.
Table from National Eating Disorders Association
Feature image: wan mohd, corridor, used under CC BY license/cropped from original