Over the past two years, the federal government has passed a series of highly-publicized anti-immigrant laws. Some of these laws limit the number of new immigrants who can enter the US legally, and prohibit immigration from certain countries. Other laws make life harder for immigrants who are already in the US—for example, by stripping legal status from migrants who are here on humanitarian programs. While it’s too early to know how these policy changes will affect our communities over the long term, they could worsen health disparities for Latinos for decades and generations to come. The courts haven’t allowed the Trump administration to implement some of their harshest policies, but these effects might emerge even if the policies aren’t implemented.
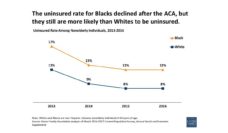
The health impacts of state and local laws that increase immigration enforcement and decrease access to services and benefits for undocumented immigrants are well-documented by researchers. In a recent study, I asked how anti-immigrant laws in ten states impacted health care access for Latino children who were born in the US to noncitizen parents, and whether these effects differed depending on characteristics of the counties where families lived.
Using ten years of data from the CDC National Health Interview Survey, I looked at how Medicaid enrollment rates changed after states passed omnibus laws. I also wanted to know if these changes in enrollment differed based on the percent of the county population who were Latino.
Across counties with anti-immigrant policies in place, Latino adults report more anti-immigrant discrimination as county Latino density increases.
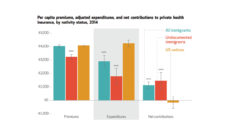
I found that law passage did not affect Medicaid enrollment for Latino children who lived in counties with relatively few Latino residents. However, as size of the Latino populations increased, the laws had harmful effects. Children in counties that were 25% Latino were 10% less likely to have Medicaid coverage after the laws passed. In counties that were 35% Latino, children were 21 percentage-points less likely to have coverage. Most of these children became uninsured. They did not move to private health insurance plans. This loss of health insurance will likely translate to worse health, lower educational attainment, and lower earnings into adulthood.
Why does living in a county with a high percentage of Latino residents place children at risk of losing Medicaid coverage when an anti-immigrant law passes? The explanation may lie in how native-born Americans react to large and growing immigrant populations. Across counties with anti-immigrant policies in place, Latino adults report more anti-immigrant discrimination as county Latino density increases. And Latinos in counties with very high concentrations are at greater risk of being deported. Both discrimination and risk of deportation discourage parents from seeking health care for their children.
So, what can local governments, immigrant advocates, and public health professionals do to promote health equity for immigrant families? Possibilities include: working with trusted community organizations to enroll eligible children in benefits. Making sure state Medicaid workers don’t ask about parents’ immigration statuses when they apply for benefits for their eligible children. And reducing barriers to transportation to program offices and clinics.
Feature image: brazzo/iStock