Accountable Care Organizations (ACOs) have been around in some form since 2005, with the Medicare Physician Group Practice Demonstration as an early forerunner to the Medicare Shared Savings Program (MSSP) which began in 2012. ACOs are growing rapidly in number of organizations and covered lives. The MSSP is a strong step in the transition to value-based care and focuses on enhancing quality, reducing costs and improving health outcomes. Many ACOs are still in their initial learning and transition phases. It takes time to realign incentives and change behavior, making it essential to refine and improve the program’s design and methodologies to ensure long-term success. With ACOs now affecting care in nearly every county of the country they are becoming ubiquitous, and with that ubiquity comes great potential to lead the healthcare industry in the transition to value-based care.

ACOs were designed to shift care orientation toward population health and bend the cost curve by incentivizing providers to be financially accountable for the entire provision of healthcare of their patients. This means in large part, coordinating and improving care transitions as patients move from one care setting to another. Under the ACO model providers take greater responsibility for maintaining and improving the health of their patients over time.
As seen in Figure 1 below, ACOs are achieving greater success over time. An increasing number and proportion of ACOs are earning shared savings payments from CMS, which requires that participants meet certain quality measure requirements and have substantially lower expenditures than expected.
Figure 1: MSSP ACOs Earning Shared Savings (number and percent), 2013-2015
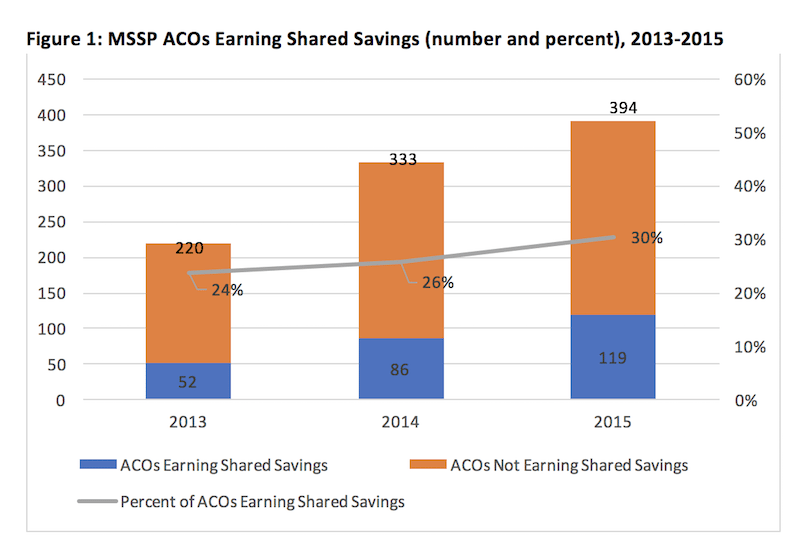
Source: Dobson | DaVanzo analysis of ACO Public Use Files for 2013, 2014, and 2015
In addition to the program improving performance as the program matures, individual MSSP ACOs appear to perform better over time. That is, compared to new ACOs entering the program, ACOs that have been in the program for three years have an 85% higher likelihood of earning shared savings.
The CMS pays more back to ACOs in shared savings than ACOs generate in savings in the MSSP. However, improved performance over time has enabled the gap between programmatic spending and savings to narrow substantially for experienced ACOs (see Table 1 below).
Table 1: Results for MSSP ACOs PY1-PY3 by Number of Years Active in Program
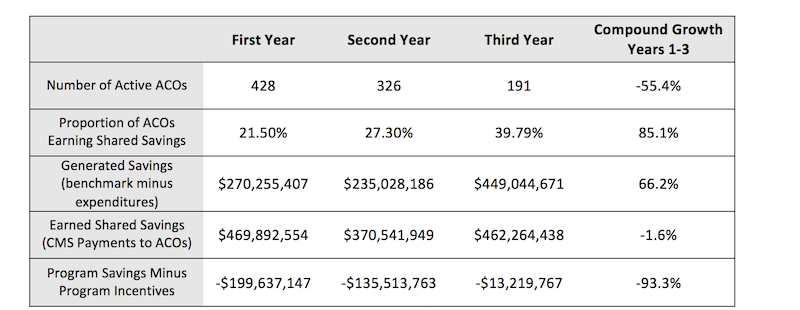
Source: Dobson | DaVanzo analysis of MSSP Fast Facts, and Public Use Files for 2013, 2014, and 2015
Discussion
The MSSP is an emerging program affecting an increasing number of patients and is resulting in providers and healthcare organizations improving the quality of care they deliver. In addition to CMS incentives, ACOs face internal pressure to achieve return on their investments that were needed to become a well-functioning ACO such as improvements in care and organizational management structure. We have found that ACOs are growing in population covered and number of ACOs and ACO financial performance has improved as they mature:
- ACO expenditures are lower than their benchmarks (in aggregate);
- Program shared savings were achieved for 30 percent of participating organizations in the most recent performance year;
- ACOs with more experience in the program earn shared savings at a higher rate; and
- The program is on the path to being self-sustaining for CMS while improving quality and access to care.
Further research is necessary to better understand the effects of ACOs. Adjusting for patient level characteristics, ACO structural characteristics and geographic location provides some insight into what drives ACO performance. Research with clinical, administrative and survey data would also be of use to study the clinical effects of ACOs.
Feature image: Herry Lawford, The City, A doctor’s consulting room, used under CC BY 2.0