Outbreaks of tuberculosis (TB), an illness commonly causing death around the globe but rarely in this country, reappeared in the U.S. as recently as the 1980-90s. Increasing TB case counts occurred with the rise of HIV/AIDS, a condition that weakens the immune system and leaves individuals more susceptible to TB.
But upsurges continue today, sometimes in settings that use congregate living. For example, in correctional facilities, many people live in close proximity, which leaves both prison populations and staff more vulnerable to transmission of TB.
Rebekah Stewart and colleagues conducted a study to analyze key characteristics of outbreaks in U.S. state prisons. To understand recent trends, they used the National Tuberculosis Surveillance System to identify cases that appeared nationwide (i.e., not limited to prison populations) between 2011 and 2019. They found more than 85,000 verified cases of TB in that time. Yet, only 566 (less than 1% of the U.S. total) were diagnosed among individuals incarcerated in a state prison.
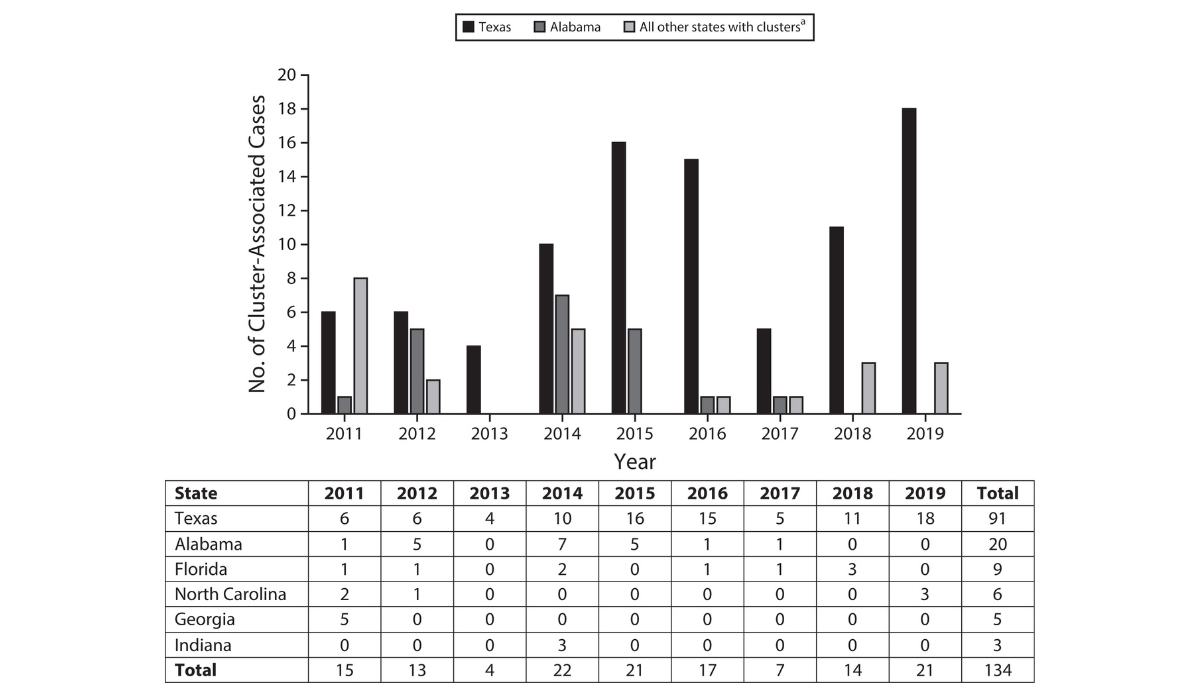
Out of these 566 cases, the authors traced those that were directly related to each other. They identified “clusters,” or state prisons that had 3+ related cases in 3 years. There were 19 clusters across 6 states: Alabama, Florida, Georgia, Indiana, North Carolina, and Texas (as shown in the Figure above). Texas and Alabama contained several larger clusters (6 cases or more). The Figure shows that outbreaks in Alabama ceased after 2017 but continued in Texas.
The research team’s analysis demonstrates that TB outbreaks in prisons are relatively rare, but they note that current surveillance data is incomplete.
U.S. state prisons could benefit from adopting strategic testing, isolation, and treatment to limit clustered outbreaks, which for Texas would mean far fewer incarcerated people sickened by tuberculosis.
Databyte via Rebekah J. Stewart, Kala M. Raz, Scott P. Burns, et al. Tuberculosis Outbreaks in State Prisons, United States, 2011–2019. American Journal of Public Health, 2022.