As Congress was pursuing its most recent attempt to repeal and replace the Affordable Care Act a few weeks ago, the Trump administration was also making headlines with its cutbacks to enrollment assistance and revelations about the use of federal funds dedicated to outreach for marketing against the ACA. On July 20, 2017, two federal contractors that support in-person enrollment assistance in 18 cities were notified by the Centers for Medicare and Medicaid Services that an option year covering the 2018 open enrollment period was not being exercised.
On the same day, it was reported that “consumer information and outreach” funding was used by the Department of Health and Human Services to develop and distribute video testimonials about “how Obamacare has harmed their lives.” Senators Schatz (D-HI), Booker (D-NJ), and Murphy (D-CT) sent a letter to Secretary Price the next day requesting information “about the apparent use of taxpayer dollars…to produce advertisements…that promote opposition to the Affordable Care Act.” There is also uncertainty about whether the administration and Congress will allocate funding made available in past years to help states encourage enrollment. Partnerships for outreach to the Hispanic community also seem to be going by the wayside. Despite the apparent political motivation behind these decisions, it is nevertheless important to understand how utilization of Marketplace enrollment assistance may have changed over time as the 2018 open enrollment period approaches.
Enrollment assistance channels
There are numerous types of in-person enrollment assistance through approximately 5,000 programs that helped consumers enroll during the 2017 open enrollment period. Use of in-person assistance was down approximately 10% over 2016 with an increasing shift toward those renewing coverage rather than enrolling for the first time. Large assistor programs—those serving more than 1,000 consumers—are shouldering a heavy load, in particular with time-intensive visits related to identity proofing and data mismatches, forcing nearly a third of them (30%) to turn away requests for help.
Less attention has been paid to the most readily available source of enrollment assistance, the Marketplace call center. The Marketplace call center is available to consumers in states utilizing the healthcare.gov platform. Total calls to the Marketplace call center and plan selections by open enrollment period were obtained from Office of the Assistant Secretary for Planning and Evaluation at the Department of Health and Human Services. These metrics capture all activity in federally-facilitated (FFM) and federal partnership (SBM-FP/FPM) states during the 2014 through 2017 open enrollment periods including subsequent special enrollment periods. The daily average call volume and calls per plan selection were calculated for each open enrollment period.
Marketplace call center volume
The total number of calls during open enrollment has declined by nearly half (–46.8%) from 2014 to 2017 as plan selections rose by more than two-thirds (69.0%) (Table 1). The elevated call volume during the 2014 open enrollment period was likely a byproduct of the issues with the initial rollout of healthcare.gov and a lack of familiarity with the enrollment process. This is reflected in an average of more than four calls per plan selection (4.35) during the 2014 open enrollment period. There was a large drop off during the 2015 open enrollment period to just under two calls per plan selection (1.90) followed by smaller declines over the last two open enrollment periods (2016–1.61, 2017–1.37), which likely reflects increasing familiarity with the Marketplace and automatic re-enrollment for many. Average daily call volume declined by approximately 30,000 during the 2017 open enrollment period relative to 2015 and 2016 but was still higher than 2014.
Table 1. Marketplace call volume and plan selections by open enrollment period
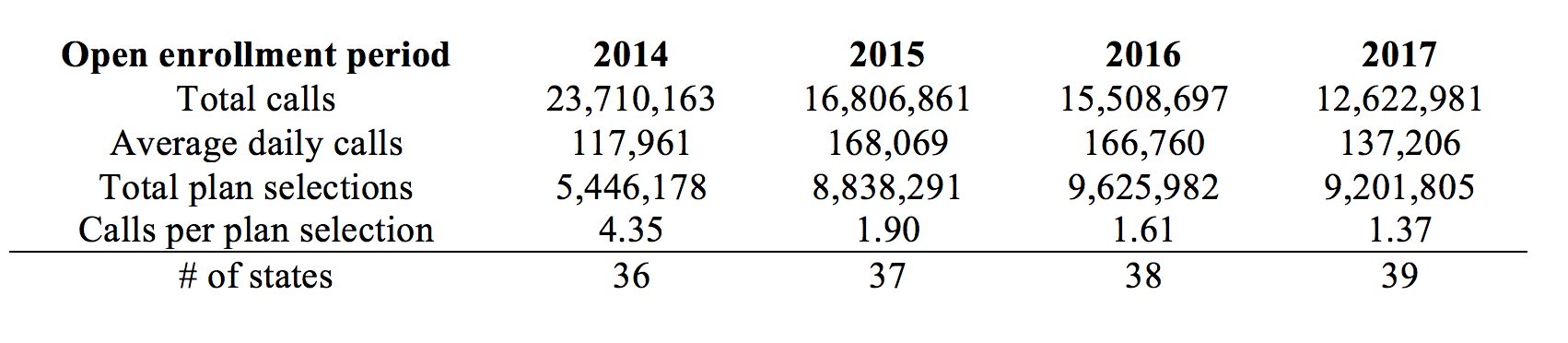
Calls per plan selection have declined with each open enrollment period but activity is still quite high—averaging more than one call per plan selection in 2017. Reductions in support for in-person enrollment assistance along with confusion among consumers fueled by political uncertainty and the counter-marketing efforts noted above could cause a rebound in call center activity, particularly if the larger volume assisters are impacted. However, in addition to the cutbacks noted earlier, federal contractors have also announced recent layoffs from call centers in Iowa and Texas that serve the Marketplace. The 2018 open enrollment period will also only be 45 days long—half the length of open enrollment in prior years (3 months)—which may place a substantial strain on declining enrollment assistance infrastructure. A rebalancing of outreach efforts may be warranted after several years of Marketplace operation but the rhetoric from the President and his administration leaves little doubt that politics—and not efficient deployment of resources—is the overriding concern behind these decisions.
Author’s note: This post was written before the announced cuts to advertising and navigators last Thursday, which apparently were a last-minute decision. Given the likely consequences of these cutbacks to engagement with the Marketplace, the motivation behind the actions cited above becomes perhaps even more clear.
Feature image: Bill Rice, Phones for GOP Victory Center, used under CC BY 2.0













