The Trump administration is prompting many of us in health services to ask new questions about if, and how, to draw lines between our personal and professional endeavors. Do we sign that petition with our institutional affiliation? Do we retweet that tweet? Do we share news of that protest on the established mailing list? As someone who studies organizational ethics, these individual-level questions soon give way to a larger set of questions about the roles and responsibilities of the institutions within which we spend so much of our professional lives. In a moment in which the role of institutions appears critically important, what does it mean to be a just institution?
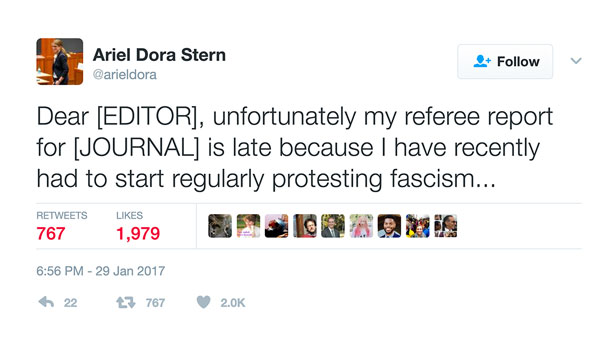
Recently, local leaders have shone light on this question. Over a weekend of protests in January, Harvard Business School faculty member Ariel Dora Stern (an expert in management of innovation in health care) imagined aloud about how to prioritize her academic responsibility to a journal and her social responsibilities to her community. The tweet accrued nearly two thousand retweets and replies from fellow faculty including “Isn’t that the truth?” and “I’m in the same boat.” One response asked whether the journal had issued a formal statement against an executive order, suggesting that if it had not, Professor Stern should no longer be willing to review.
More recently, former President and CEO of the Institute for Healthcare Improvement drew attention on STAT News by calling for Dana Farber Cancer Institute to cancel or move the fundraiser it has planned at Donald Trump’s Mar-a-Lago resort. He wrote, “Dana-Farber leaders say they want to “stay out of politics. But this is a time when inaction is every bit as political as action.”
The question of what it means to be a just institution may be particularly tricky for organizations premised, in varying ways, on the improvement of health. An organization that makes widgets may be able to draw a clear boundary around its production process and ask employees to take up political matters when they are “off the clock.” Arriving at similar clarity in organizations vested in health seems impossible.
First, the breadth of health’s definition and the diffuseness of its roots allows any action (at the individual or institutional level) to be examined through the lens of its health impact. Everything is implicated in the health production function, including the social and political conditions that have been threatened by this Administration.
Second, many of us see our work in health as a vocation, rather than a job. Even among those of us who work clearly defined shifts, our professional identities stay with us in off hours and in many cases, well into retirement. And we know that the trappings of these identities – white coats, access to public platforms, power over substantial resources – are valuable as symbols and tools. In sum, when it comes to creating health, both the work and our roles are poorly bounded. This leaves institutions, which operate on the basis of formal rules and structures, in a difficult position.
My hope is that as health institutions – hospitals and clinics, professional associations, schools, government agencies – people in leadership positions will lean into these conversations rather than away from them.
Academic institutions face additional challenges. At public health and medical schools, the administration is generally expected to create and protect a sense of community wherein students, in particular, feel safe and represented. Operationalizing this expectation is no easy task. To what extent should administrators create platforms for student advocacy versus protect students from triggers and burnout? More generally, organizations with a focus on learning must work to preserve of an environment that can hold conflicting views. As a result, the burden falls to institutional leadership to decide when to support productive dissent versus when to stamp out bigotry. And of course, the commitments to foster community and promote learning can compete, if not conflict, with one another.
None of these questions can be answered simply. Each requires us to get back to first principles of who we are as individuals, what we stand for as institutions and how we can best respond to upheaval. My hope is that as health institutions – hospitals and clinics, professional associations, schools, government agencies – people in leadership positions will lean into these conversations rather than away from them. Such a dialogue may well be messy, but the key will be to recognize the messiness as a feature of, rather than a bug in, the process.
Alongside these conversations, I suspect that some deadlines will continue to be missed, colleagues are likely to say inartful things, and administrators may under- or over-react to political happenings. I would urge us to remember that we in health have always been a community inclined towards moral justice – and in most cases, we are all doing the best we can to realize that commitment in a new environment. Thus, let us exercise an ethic of forgiveness. Doing so inside our institutions can both buy us some time to wade through these complexities together and allow us to practice being the change we wish to see in the world.
Feature image: Joe Piette, Feb 4 anti-Pence protest, used under CC BY-NC 2.0