Human papillomavirus (HPV) is a sexually transmitted infection so common that nearly all sexually active men and women in the United States will get HPV at some point in their lives. Most people never develop symptoms and their HPV infection goes away on its own, but sometimes infection can lead to serious problems. HPV is associated with cervical, anal, and oropharyngeal cancers (back of the throat, including the base of the tongue and tonsils) and accounts for approximately 31,500 new cancer cases in the United States each year.
Fortunately, an HPV vaccine has been available since 2006 that can reduce the risk of HPV infection and associated cancers.Currently, the Centers for Disease Control and Prevention (CDC) recommends that all 11- and 12-year-old adolescents receive two doses of the HPV vaccine over a six to twelve-month period.
Studies have estimated that the HPV vaccine may prevent 29,100 cancers each year. Despite its effectiveness, HPV vaccination rates remain substantially lower than rates for other vaccines routinely recommended for adolescents. Studies have identified several barriers to HPV vaccination, primarily parental concern, lack of knowledge, and mixed opinions regarding HPV vaccination. These include opinions that the vaccine encourages risky sexual behaviors or should be administered after onset of sexual activity (when it is no longer as effective) and concerns about HPV vaccine safety.
Currently, the Centers for Disease Control and Prevention (CDC) recommends that all 11- and 12-year-old adolescents receive two doses of the HPV vaccine over a 6-12-month period.
Improving HPV vaccination is critical for reducing HPV-associated infections and cancers. The National Committee for Quality Assurance (NCQA) conducted a study to learn about health plan strategies for improving HPV vaccination. We interviewed a subset of commercial and Medicaid health plans who had relatively higher rates of HPV vaccination coverage among female adolescent plan members. Despite existing barriers to HPV vaccination, there are common strategies that health plans can implement to achieve higher HPV vaccination rates.
“Normalize” HPV vaccination
A critical strategy for improving HPV vaccination rates is to “normalize” HPV immunization during adolescent well-visits. This involves helping parents understand that the HPV vaccine is a normal part of adolescent immunization, rather than an optional vaccine. Plans should encourage providers to offer all three recommended adolescent vaccines at the same well-care visit. Plans and providers can also emphasize that the HPV vaccine is recommended for good health and important for cancer prevention both in educational materials and in conversations with patients.
Educate patients and providers
Patient and provider education is integral to supporting HPV vaccination. Plans can use Web sites, written materials/pamphlets, newsletters or other resources to disseminate information to providers and patients. The plans we interviewed emphasized that educational materials were more meaningful to patients when they cited recognized sources (e.g., the CDC or the American Cancer Society).
Provide reminders to patients
Plans can use automated phone calls or texts to remind patients of appointments for subsequent doses of vaccine after the initial dose or send postcards and letters stating the next vaccination due date.
Provide feedback to providers
Plans can also use automated reminders for providers or send them reports of patients who have not yet completed the HPV vaccine series. Moreover, plans can share performance data with providers, such as reports about their patients’ immunization rates compared to other providers in the plan. This effort may inspire healthy competition among providers that increases vaccination rates overall.
Increase access to registry data
Multiple plans stated that access to a state immunization information system (IIS), also called an immunization registry, is useful for tracking vaccinated patients. An IIS is a confidential, population-based, computerized database that records all immunizations administered by participating providers to persons residing within a given geopolitical area. Laws regarding the operation of IIS systems vary by state. Policies that facilitate the use of state IIS systems and data exchange are important for plans and providers to track accurate immunization information and keep adolescents up-to-date on vaccines.
Overcoming parental concerns regarding the HPV vaccine and the stigma surrounding its connection to sexual activity remain important challenges. Additional actions beyond what is described here are likely needed to achieve optimal HPV coverage. However, these findings suggest a starting point for a larger discussion about strategies to support HPV vaccination for all adolescents.
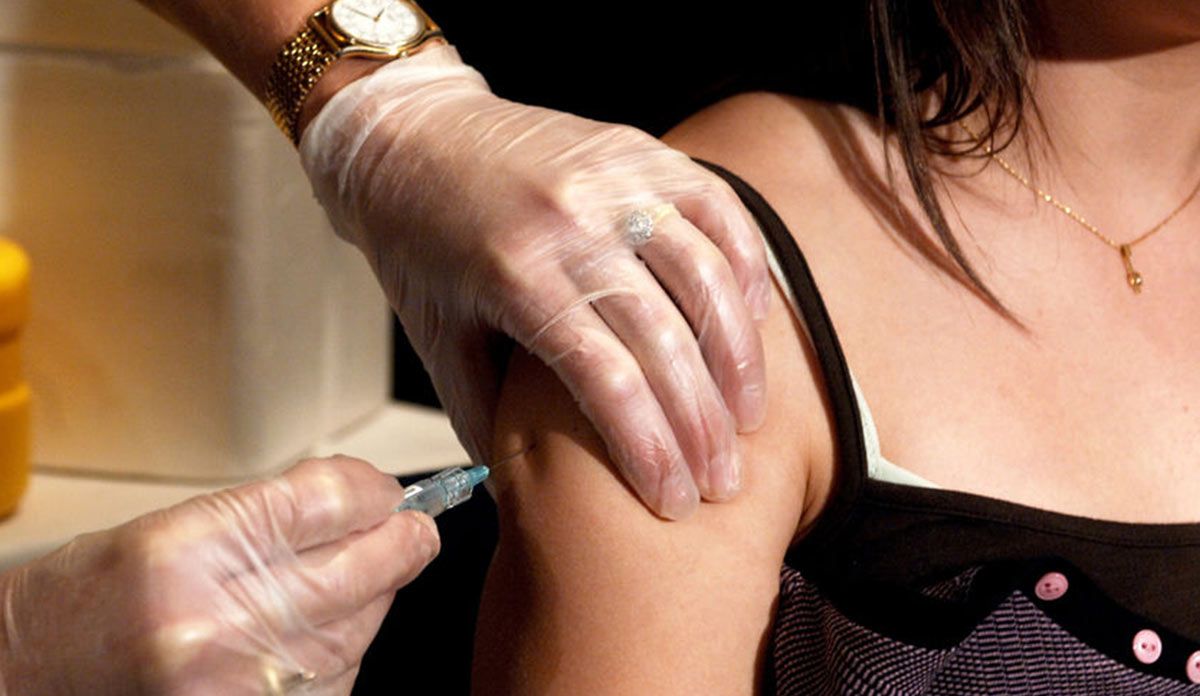
Feature image: VCU CNS, hpv vaccine, photo: Art Writ, used under CC BY-NC 2.0