One of the most controversial challenges when responding to humanitarian emergences is the diagnosis and management of psychological trauma in general and more specifically post-traumatic stress disorder (PTSD). The questions most frequently debated are: Does diagnosis truly capture the psychological suffering of refugees? Or, does it pathologize normal reactions to disaster? Some also argue that applying diagnostic checklists too early after a mass trauma event may generate artificially high estimates of PTSD.
In the refugee context, people are exposed to both repeated and ongoing traumatic triggers (fear from the past, current uncertainties, new traumas). This means that the classic PTSD model of one trauma then lengthy recovery is the exception rather than the rule.
“Trauma is a multidimensional experience of mostly targeted rather than random occurrences, which is situated within a social context and a temporal sequence.”
A large meta-analysis concluded that mental health problems among refugees are not always a direct consequence of their acute traumatic stress, and may be a reflection of their experiences after displacement. Stressors and symptoms may differ at each stage of a refugee’s journey (pre-migration, migration, post-migration, or resettlement).
The prognosis of classic PTSD has as much to do with events that occur after the trauma as with the trauma itself. For example, the onset and duration of PTSD among survivors of hurricane Katrina was largely explained by gender, financial situation, social support, and post-disaster events such as physical and sexual assault. In particular, lack of social support has been identified as a primary risk factor for developing PTSD. Research has shown that it is essential to reduce isolation and maintain connection with extended family and a sense of “moral dignity” while in exile. This definition of “trauma” by Suarez captures all of these elements: “Trauma is a multidimensional experience of mostly targeted rather than random occurrences, which is situated within a social context and a temporal sequence.”
Overemphasizing trauma at the expense of strength may affect how practitioners view their therapeutic task and create a barrier to full recovery by undermining patients’ ability to survive adversity.
It is common for mental health professionals working with refugees and displaced people to focus on the “trauma story,” often at the expense of what allowed these people to survive (i.e., their resilience). This has important consequences as it may result in strengths being overshadowed by a “deficit model” that depicts people who have experienced displacement as traumatized victims. Overemphasizing trauma at the expense of strength may affect how practitioners view their therapeutic task and create a barrier to full recovery by undermining patients’ ability to survive adversity.
In addition, focusing on the psychological aspects of the traumatic event (as important as it is to our work) may overlook the ways in which trauma is mediated by political and religious convictions, cultural beliefs, social circumstances, and previous experiences with adversity.
The term “humanitarian emergency” carries a certain danger with it, since it implies that the solution lies largely within the “humanitarian assistance” domain while overshadowing contextual factors that may shape mental health outcomes. Ultimately, psychological recovery comes from improvements in the overall political, economic, and societal circumstances and the meaning people find in their lives, and not simply from resolving their traumatic stories.
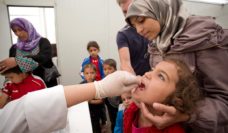
Feature image: Syrian refugees in Adana, Turkey. © 2016 TERsaci/photography collective, courtesy of Photoshare.