Medicaid was introduced in the 1960s to address health care financing among low-income populations. Public health research in subsequent decades illuminated social and economic factors impacting health above and beyond the ability to pay for health care services. For example, people experiencing homelessness face trouble staying safe, keeping track of medication supplies, and unsanitary living conditions — barriers to health. Although Medicaid provided the means to pay for healthcare, it did not address other important drivers of health beyond the ability to access care.
The 2013 implementation of the Affordable Care Act enabled states to address barriers to health by applying for special waivers to experiment with how they used Medicaid funding. With an understanding of powerful social and economic predictors of health, some states applied for waivers to fund housing support services for people experiencing homelessness. For example, the state of New Jersey expanded housing support services under Medicaid to the state’s over 10,000 residents. Few studies have examined whether providing stable housing leads to changes in Medicaid-funded health spending among this population.
Joel Cantor and his team examined the relationship between Medicaid health spending and permanent housing support services in the state of New Jersey. Specifically, they identified 8,400 people eligible for permanent housing support and tracked this group’s use of Medicaid and housing services.
To address the needs of all people experiencing severe homelessness in New Jersey, the researchers estimate that the state would need to double the number of available resources such as housing subsidies and the number of houses available.
Half of participants in the sample were already receiving Medicaid-sponsored housing. The researchers categorized the remaining half into three groups based on length of history of homelessness and disabling medical conditions, such as HIV, mental health-related problems, and developmental disabilities.
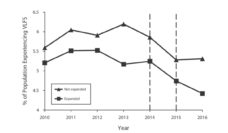
Compared to those currently enrolled in Medicaid-supported housing, people with the shortest histories of homelessness spent 10% more on health services than those with stable housing. The participants with the longest histories of homelessness and the most disabilities spent 27% more on healthcare than those with stable housing. This number represents as much as $5,727 more annual spending on Medicaid-sponsored healthcare.
Providing Medicaid-sponsored housing results in health-related savings. Greater investments in Medicaid-supported housing could lead to large reductions of spending on expensive and avoidable hospital services for those experiencing chronic homelessness.
To address the needs of all people experiencing severe homelessness in New Jersey, the researchers estimate that the state would need to double the number of available resources such as housing subsidies and the number of houses available. Current waivers for Medicaid-supported housing do not allow for greater funding for these resources and would require new Medicaid rules to have the widest effects.
Photo via Getty Images