One in six mothers are being shouted at, scolded, or threatened during childbirth in the US. Mistreatment can also manifest as disregard for mothers’ preferences or mothers receiving no response to requests for help.
In a recent study, titled Giving Voice to Mothers, researchers analyzed mistreatment by race, age, immigrant status, and socio-economic status. In a survey of 2,138 women, mistreatment was characterized as physical, sexual, or verbal abuse, neglect and abandonment, poor rapport between women and providers, loss of confidentiality, and lack of supportive care. Researchers also examined mistreatment by place of birth (at home, in a hospital, or in a birthing center), mode of delivery (vaginal or caesarian), and type of provider.
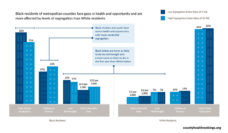
Women of color were twice as likely to be ignored or refused requests for help by healthcare providers as White women. This is particularly alarming because delayed response to clinical warning signs is the leading cause of maternal mortality in the US, especially for African American mothers. This was the case for Kira Dixon Johnson, who bled to death following the birth of her son because health care providers waited 10 hours before attending to her requests for help. Regardless of maternal race, having a Black partner increased reported mistreatment. White women with a White partner reported the least mistreatment (12%).
Immigrant mothers were more likely to report mistreatment than their US-born counterparts, as were younger women and first-time mothers. Women with low socio-economic status were twice as likely to report being threatened or shouted at by health care providers compared to women with moderate or high socioeconomic status. Women with pregnancy complications and women with a history of substance use, incarceration, or intimate partner violence reported the highest overall mistreatment rates.
This is particularly alarming because delayed response to clinical warning signs is the leading cause of maternal mortality in the US, especially for African American mothers.
Experiences of ill treatment differed significantly by place of birth. Five percent of women who gave birth at home experienced mistreatment compared to 28% who gave birth in a hospital. Violation of physical privacy was three times more common in hospital settings. The likelihood of being ignored or refused help was more common among women who gave birth in hospital settings (13%) than those who delivered at home (with the help of a midwife or doula) or in a freestanding birth center (2%).
Finally, mode of birth was also correlated with reports of mistreatment. Higher rates of mistreatment were reported among women who had unplanned caesarians than those who had vaginal births. Women who had prenatal care from midwives were much less likely to report mistreatment compared to those who had prenatal care from physicians.
Understanding women’s lived experiences during and after pregnancy is essential to optimize birth outcomes. Findings from the Giving Voice to Mothers study highlight settings, institutional practices, and racial disparities that need to be improved in maternity care, for the dignity and health of the mother and well-being of her child and family.
Image by Gordon Johnson from Pixabay