The list of disparities in health care outcomes is long, with many stemming from systemic racism, low income, and economic and insurance status. These disparities became painfully obvious when socially marginalized Black and Brown individuals and populations bore the brunt of illness and death during the COVID-19 pandemic. Studies have now shown that individuals living in historically disadvantaged areas continue to experience the residual effects of long-time discriminatory practices.
We have known for decades that low-income levels stand in the way of good health care. Discovering the obstacles that contribute to this key disparity is critical to figuring out how to minimize them. Although fair access to high-quality health care for all people is crucial for preventing and treating illness, not everyone in the United States has equal access. One factor that can help determine the level of access to health care among people with low income is the distance between their home and a health care facility.
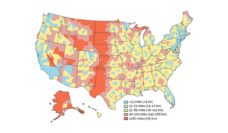
In a collaborative study between the University of Florida, the University of California at San Diego, and the University of Pittsburgh, my colleagues and I investigated the degree to which driving distance to the closest health care facility played a role in preventing equitable health care access for people across the United States. We compared the travel distances to the nearest facility in 1,166 metropolitan counties and in 1,967 non-metropolitan counties between low-income (less than 200% of the federal poverty level) and other residents.
Low-income residents had a significantly higher likelihood of needing to travel more than 10 miles to the closest facility in rural areas and more than a mile in urban areas. Our findings suggest that low-income residents have worse access to health care. The high prevalence of this structural disparity may perpetuate the unfair poor health care outcomes, including cardiovascular emergencies, for U.S. residents with lower income levels.
Although multiple sociodemographic factors and obstacles to health care access must also be determined and addressed, geographic barriers are particularly important for individuals with low incomes because they are less likely to own a car and more likely to live in areas with lower access to public transportation.
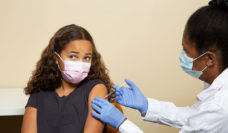
Photo via Getty Images