Access to high-speed internet is now thought of as a fundamental part of life and social functioning that influences economic opportunity, health, and quality of life. Because we depend on the internet for so many parts of life – from finding employment to managing finances and health – quality access is increasingly considered to be a social determinant of health.
Use of new health technologies often requires internet access. One common example is the growing availability of electronic patient portals (also called personal health records). A patient portal is an electronic system that lets patients directly interact with their doctors or nurses 24 hours a day on a computer, tablet, or smartphone. Patients can easily view their personal health information (e.g., current medications, lab results, vaccinations), schedule appointments, and actively participate in their own health care.
Research suggests that both patients and healthcare providers benefit from patient portals. Research also shows, though, that socially disadvantaged patients are less likely to use patient portals despite being interested in such technology to improve their healthcare experiences.
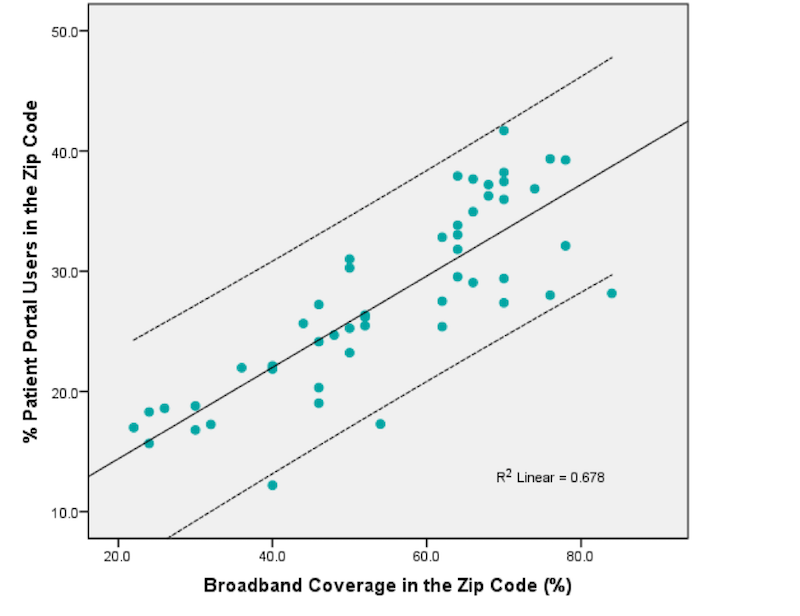
In order to better understand barriers to using patient portals, we studied the usage patterns of over 243,000 patients from a public healthcare system in Cleveland, Ohio who had made at least one outpatient appointment from 2012 to 2015. During those years, about 30% of patients had used the patient portal system at least once, and White patients were more likely to use the portal compared to African American and Hispanic patients. Notably, we also found that, as the percentage of home broadband connections in an area increased, so did the percentage of patients using the portal (see Figure 1). In neighborhoods where 20% or fewer residents had home broadband connections, only 17.5% used the patient portal, compared to 35% of patients who lived in fully connected neighborhoods.
In response to these findings, we are currently analyzing data from a related study to evaluate the effectiveness of a digital literacy training program facilitated by community health workers (CHWs). From August 2017 to January 2018, patients met with a clinic-based CHW who explained patient portal use, gave brief pointers, and facilitated referrals for a free, health-focused digital-literacy training program. Early analysis of the data shows that, based on clinical records from 6 months before and 6 months after implementation, the CHW program was associated with a three-fold increase in the rate of first-time patient portal use and double the rate appointments scheduled using the portal. Reluctant patients described high cost and anxiety about the internet as the most common barriers, while enthusiastic patients stressed the convenience of fast access to lab results, messaging doctors, and having family members’ health information in one centralized location.
Although healthcare organizations and community-based digital inclusion programs can work together to overcome social and technological disadvantages, over 24 million Americans do not have high-speed internet. A study by the Connect Your Community Institute using Federal Communications Commission data found that Cleveland’s lower-income, predominantly African American neighborhoods were systematically excluded from broadband networks.
In combination, these findings suggest that many people in the United States are being excluded from using modern tools to participate in their own healthcare. A combination of community-based training partnerships and policy changes are necessary to reconcile these differences in digital access and eliminate barriers to healthcare and communication with providers.
Feature image: J.C. Burns, More fiber in our diet. Used under CC BY-NC-ND 2.0.
Graph from Perzynski AT, Roach MJ, Shick S, Callahan B, Gunzler D, Cebul R, Kaelber DC, Huml A, Thornton JD, Einstadter D. Patient portals and broadband internet inequality. J Am Med Inform Assoc. 2017;24(5): 927-932.














