Every day, approximately 130 Americans die from an opioid overdose. Naloxone, an opioid reversal medication, gives us the ability to save their lives. As the United States continues to struggle with its addiction epidemic, one challenge has been ensuring this life-saving drug is available to anyone who needs it.
Think of naloxone as a fire extinguisher or a defibrillator, a tool for survival that the public needs to find and use in an emergency. To maximize effectiveness, there are two important considerations: knowledge on how to use the product and availability.
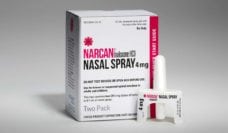
Family, friends, other drug users, or strangers who observe an overdose in public often play a crucial role. Ensuring these bystanders are able to administer naloxone is essential. One study showed nasal naloxone, the most common form, can be properly delivered by trained potential bystanders in 98% of overdose cases. The nasal spray is easy for even untrained people to use.
All 50 states have passed laws and spent money on expanding access to naloxone. All but three provide legal protection for bystanders administering the medication through Good Samaritan laws. But these efforts don’t guarantee that naloxone will be in the right place, at the right time. To improve community usage, Dr. Geoffrey Capraro, an emergency room physician, and Dr. Claudia Rébola, an industrial design expert, teamed up to design the NaloxBox in 2014. Each box holds naloxone, a CPR mask, and educational materials created by the team.

In 2017, the project received financial support from the Rhode Island Department of Health and NaloxBoxes were installed in 56 locations statewide, including homeless shelters, soup kitchens, libraries, and city halls. Naloxone was provided by the state and Capraro’s team trained employees at those locations in how to use it.
“Our first partners knew they were serving clients who were at risk for overdose,” says Capraro. “It was an easy sell, partly because we offered our product for free. But more importantly, we also all shared the same goal: reducing preventable deaths.”
Soon after the initial round of NaloxBoxes were installed, national demand quickly outpaced supply. To manage nationwide distribution, the Rhode Island Disaster Medical Assistance Team (RIDMAT), a local non-profit, assumed control of the program. Erin McDonough, a program director at RIDMAT, notes that NaloxBox is truly a “community-based initiative to address a nationwide crisis.” Local high school students designed new graphics, college students supervised printing, and now individuals in addiction recovery complete assembly of the NaloxBox itself and shipping.

Given insurance and liability concerns, RIDMAT determined they could not ship the new NaloxBoxes with naloxone included. However, Capraro believes that those ordering the product will likely have the necessary relationship with their state or health departments to obtain the medication and fill the box with its required antidote.
In February, RIDMAT began accepting orders on their website; within three weeks, organizations in Rhode Island, New York, and California bought nearly 60 units, each costing several hundred dollars. Rébola also plans to bring 36 NaloxBoxes to the University of Cincinnati, where she works.
“We need to change the narrative around bystander treatment,” Capraro explains. “The NaloxBox is part of having an open conversation about [the opioid epidemic] instead of sweeping it under the rug. We really view the box as a primary platform for disseminating information and linking people to care.”
Photo by Michael Schiffer on Unsplash