The history of HIV in the United States is riddled with stigma and discrimination, notably reflected in the longstanding restrictions preventing sexual minority men from donating blood. From 1977 until 2015, sexual minority men and their partners were not allowed to donate blood due to heightened fears of HIV transmission through blood transfusions.
In 2016, the previously indefinite ban from donating was lessened to a deferral period based on sexual history. Men who abstained from sex with other men for 12 months were eligible to donate. The Vitalant Research Institute compared the HIV infection rates of donated blood from before and after the 2016 policy change to see if the broadened donor eligibility increased the risk of HIV transmission.
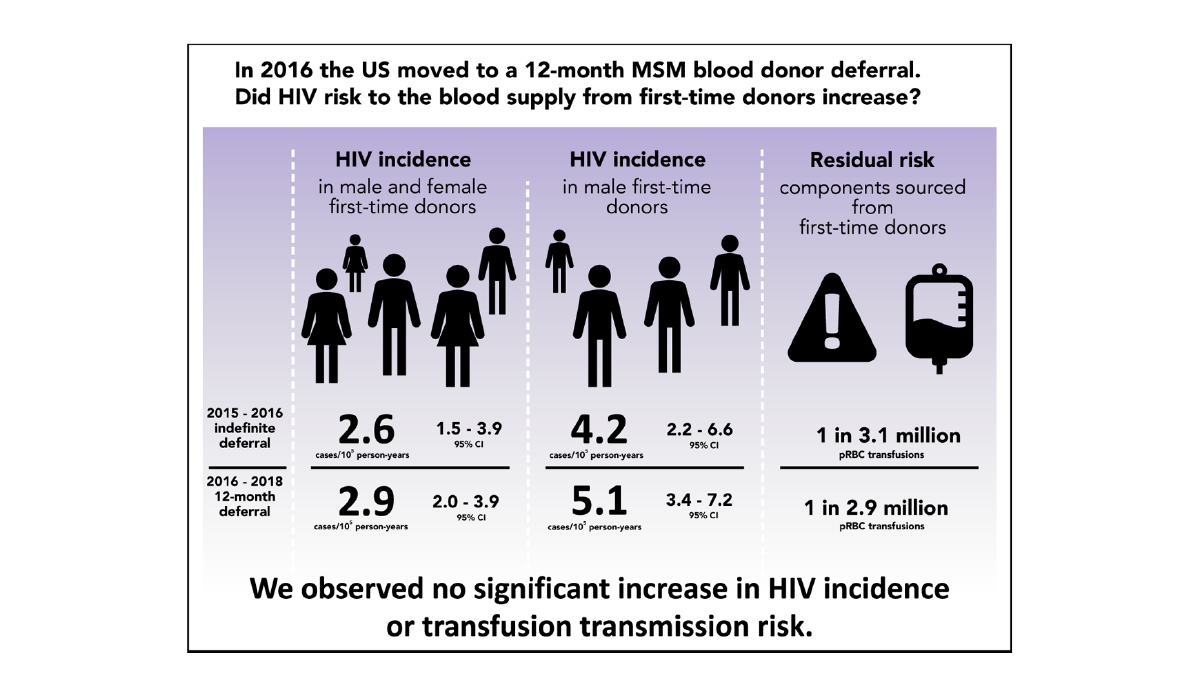
As the figure shows, the study found that lifting the restriction did not lead to an overall increase in HIV present in donated blood. In fact, donors infected with HIV were more likely to be returning donors rather than first-time donors brought in after the policy change. This finding suggests the previous restriction had not played an active role in preventing transmission of HIV infection.
There is no scientific basis for a deferral period of any length of time, for anyone. Donated blood is now tested prior to transfusion so transmission of HIV to a recipient is unlikely even if a donor is unknowingly infected through sexual activity. Policies that prohibit anyone from donating based on their sexual orientation and history are not only arbitrary, they are discriminatory. Although sexual minority men continue to have higher rates of HIV infection than the general population, they are not the only demographic with an increased risk. They are, however, the only group restricted from donating.
The Covid-19 pandemic depleted the US blood supply and as a result motivated the FDA to further lessen the deferral period to three months in April 2020. Researchers and policymakers question why the US continues to reduce the restriction and are instead pushing for the complete removal of the regulation. The current evidence illustrates that doing so poses no increased threat of HIV infection and could instead save countless lives.
Databyte via Grebe E; Busch MP; Notari EP; Bruhn R; Quiner C; Hindes D; Stone M; Bakkour S; Yang H; Williamson P; Kessler D; Reik R; Stramer SL; Glynn SA; Anderson SA; Williams AE; Custer B. HIV incidence in US first-time blood donors and transfusion risk with a 12-month deferral for men who have sex with men. Visualization by Tasha McAbee.