Until recently, Massachusetts had one of the top state housing assistance programs in the United States for displaced families and children. In 2012, however, the state’s housing policy underwent changes, requiring shelter-seeking families with children to provide evidence they have stayed somewhere “not meant for human habitation.” Other eligibility criteria for shelter intake include having faced domestic violence, natural disasters, and no-fault eviction. Emergency rooms offers not only safety, but also discharge papers that could count as such proof of housing needs.
Kanak and colleagues recently observed how often children and young adults used the emergency department as shelter, comparing trends before and after the 2012 policy change. The researchers used medical records of youths below age 21 who visited a Boston hospital’s pediatric emergency room between Sept. 2011 and Aug. 2016 and complained of or were billed for homelessness.
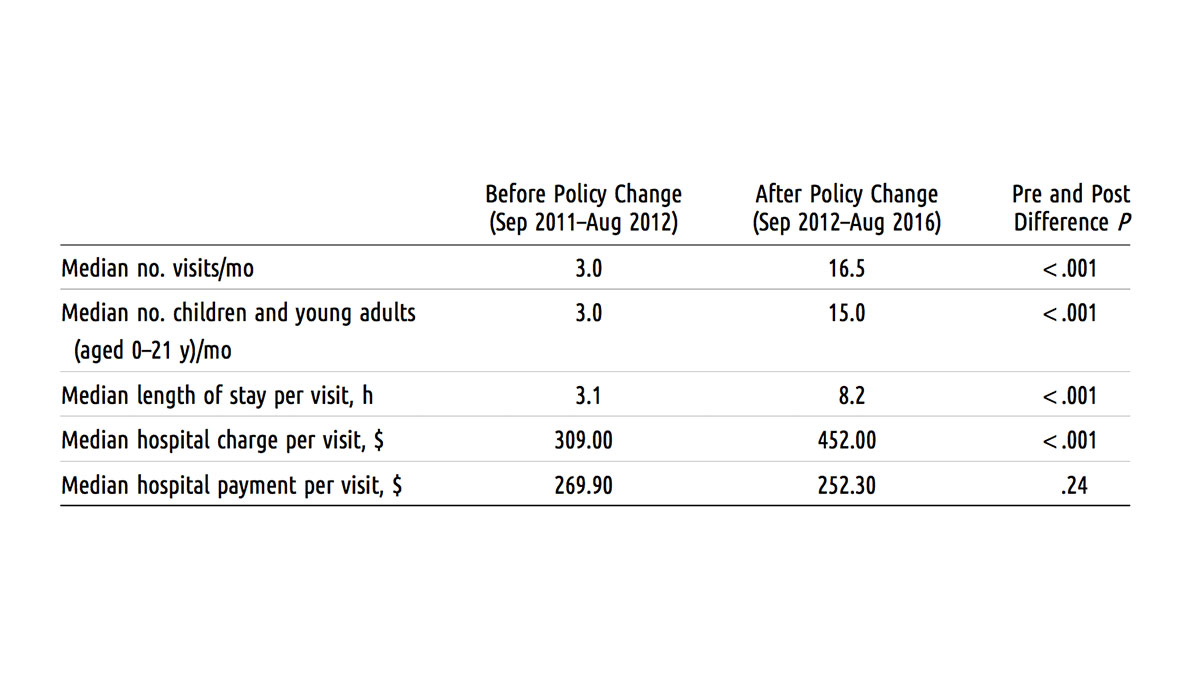
As the figure above depicts, they found the median visits per month increased drastically from three visits before the policy change to 17 visits after the policy change. Most of the children observed were 12 years or younger. The emergency department’s costs and total hospital charges over the five-year period summed to nearly $580,000; only about $19,000 of that amount accrued before the policy change.
The researchers also found that more than 8,500 emergency department hours and $200,000 of Medicaid funds were used, and they suggest that this money would have been better spent to fund housing solutions. The University of Illinois Hospital, for example, helps displaced people who continuously present to the emergency department by paying their rent.
Databyte via Mia Kanak, Amanda Stewart, Robert Vinci, Shanshan Liu, Megan Sandel, Trends in Homeless Children and Young Adults Seeking Shelter in a Boston Pediatric Emergency Department Following State Housing Policy Changes, 2011–2016. American Journal of Public Health (AJPH).