Are Hospitals Spending Enough on the Community?
Do nonprofit hospitals invest enough in community health initiatives to compensate for tax exemption status? New research shows spending on community health benefits remained essentially unchanged between 2010 and 2014.
Read Time: 2 minutes
Published:
Nonprofit hospitals are tax exempt in exchange for providing benefits to the communities where they are located. These exemptions allow nonprofit hospitals to keep $24.6 billion a year. One debate within the health policy community is whether these nonprofit hospitals invest enough in community health initiatives to compensate for exemption status.
A recent study by Gary Young and colleagues of the Center of Health Policy and Healthcare Research used data filed with the IRS by nonprofit hospitals to track spending on patient care benefits and community health. Patient care benefits include spending on financial assistance, unreimbursed costs for implementing government programs, and subsidized health services. Community health benefits are nonclinical initiatives that target social determinants of health. For example, Kaiser Permanente gives out HEAL grants to organizations that promote or offer healthy food and physical activity in underserved communities.
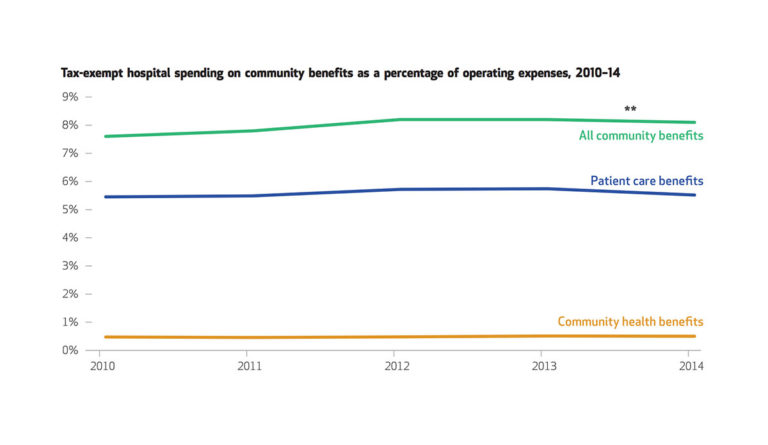
The graph above shows that spending increased from 7.6% to 8.1% from 2010 to 2014 after the implementation of the Affordable Care Act (ACA). However, the increase was mainly driven by spending on patient care benefits between 2010 and 2012 whereas spending on community health initiatives remained essentially unchanged during the four years.
The ACA tried to improve population health by requiring nonprofit hospitals to conduct community health needs assessments. The objective of these assessments was to encourage hospitals to invest more in initiatives to prevent illness and improve community health as a means of reducing expenditures on direct patient care. But this shift in spending did not happen. This data shows that hospitals continue to focus their spending on patient care rather than on programs that address community-wide public health challenges.
Databyte via Gary J. Young et al., Community Benefit Spending By Tax-Exempt Hospitals Changed Little After ACA. Health Affairs.



