Global Disruption of Antibiotic-Resistant Bacteria
The World Health Organization has sounded the global alarm calling attention to the threat of antimicrobial resistance (AMR). Given the ease of global travel, AMR bacteria can easily spread intercontinentally.
Read Time: 3 minutes
Published:
It has been over three years since the World Health Organization sounded the global alarm calling attention to the threat of antibiotic resistance, or antimicrobial resistance (AMR). National Action Plans have been sketched out in 85% of countries. Only 5% of those plans, however, are multifaceted, well-funded, and monitored sufficiently enough to address the severity of the threat. Lacking the necessary resources, many countries’ Action Plans are stalled in preliminary phases.
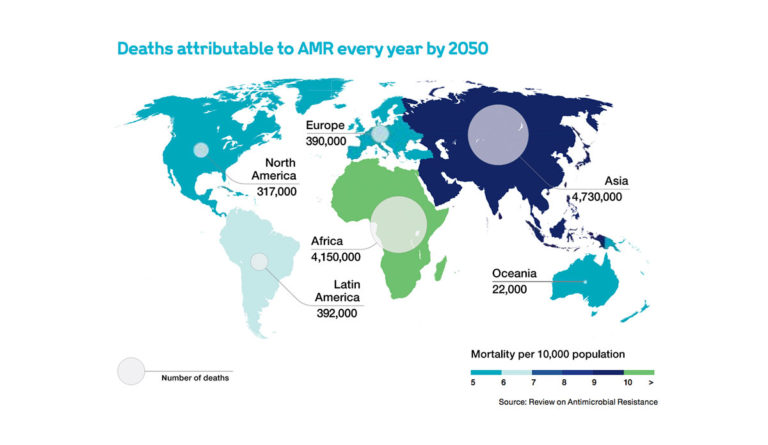
Using data from the Review on Antimicrobial Resistance, a September 2017 report from the United Nations Foundation and the Wellcome Charitable Trust helps to visualize the death toll of antimicrobial resistance by 2050. The data show extreme geographical disparity in prevalence of AMR. The mortality per 10,000 people due to AMR in Africa and Asia would be nearly twice that of the mortality in North America, Europe, and Australia by 2050. Currently, “drug-resistant infections cause around 700,000 deaths worldwide each year,” according to the report.
Antibiotic use in massive livestock operations—over 60,000 tons per year worldwide—spawns AMR bacteria, which can then be transmitted to humans.
AMR is caused by inappropriate antibiotic use on both ends of the spectrum—both excessive use and lack of accessibility are known to contribute to the burgeoning trend. And humans are not the only species affected. Antibiotic use in massive livestock operations—over 60,000 tons per year worldwide—spawns AMR bacteria, which can then be transmitted to humans.
Several antibiotic strains have emerged across the globe—from India and China to Europe and South Africa. Tuberculosis, gonorrhea, and E. Coli are three of many conditions known to have considerable resistance to various treatments.
The report calls for a global response. Given the ease of global travel, AMR bacteria can easily spread intercontinentally. Higher income countries would be wise to begin or to continue assisting their lower-income counterparts in mobilization against AMR. Various business sectors can collaborate and innovate. The food industry for one, can have a major impact. So far in 2017, even fast food restaurants like McDonald’s, KFC, Burger King, and Taco Bell have pledged to remove “antibiotics important to human medicine” from their supply chains. Others like Panera Bread and Chipotle have implemented policies against antibiotic use.
“While countries must be in the driver’s seat,” said Director of Wellcome, Dr. Jeremy Farr, “it is incumbent on all of us, across all sectors, to work together to address this challenge.”
Databyte via Sustaining Global Action on Antimicrobial Resistance. United Nations Foundation and Wellcome Charitable Trust.



