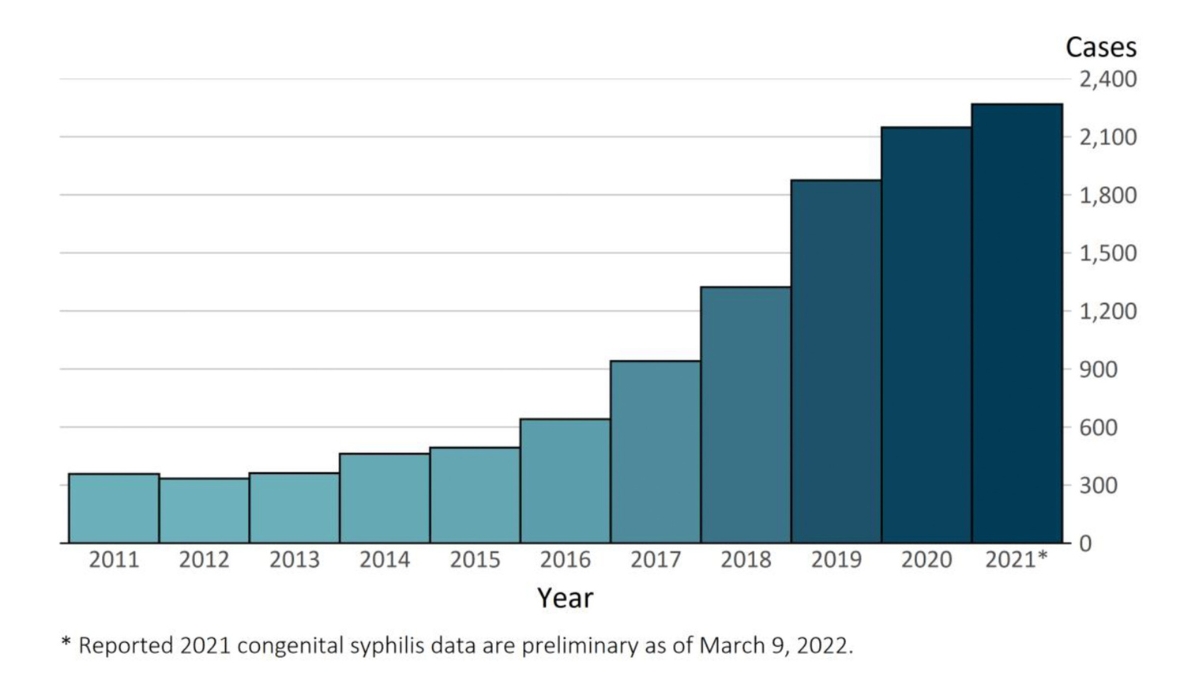
Effective treatments for syphilis have been around for seventy years, yet syphilis rates have steadily risen since 2001, particularly among reproductive-age women. This has resulted in increasing rates of congenital syphilis (CS), a condition where a fetus contracts the syphilis infection from the mother during pregnancy. This prenatal infection can lead to pregnancy or birth complications, including stillbirth, preterm birth, and miscarriages. Forty percent of newborns diagnosed with a symptomatic infection can develop neurodevelopmental delays, seizures, skin rashes, and blistering.
CS rates have increased notably since 2011, as shown in the figure above. Catherine Eppes and colleagues track this increase, and they discuss the current treatment and testing of CS. They note that the rise of CS cases may, in part, be due to the correlation between opioid and methamphetamine use in women of reproductive age and syphilis.
According to Eppes and colleagues, the diagnosis and treatment of perinatal syphilis is complex and often misinterpreted. For example, a separate study found that 25% of mothers with syphilis between 2014 and 2017 were improperly treated, and 15% were misdiagnosed as false-negative CS cases. Because asymptomatic cases of CS at birth make up 60% of all cases, these misinterpretations and misdiagnoses add to the challenges of perinatal syphilis management. Compared to those who received syphilis treatment, untreated pregnant persons are 12 times more likely to experience adverse pregnancy outcomes.
The researchers’ recommendations to improve syphilis tracking and management during pregnancy include nationally mandated syphilis screening and expanding access to syphilis databases. Increased awareness of congenital syphilis is necessary to address this continuing problem for maternal and child health in the United States.
Databyte via Catherine S. Eppes, Irene Stafford, Martha Rac. Syphilis in Pregnancy: an Ongoing Public Health Threat. American Journal of Obstetrics and Gynecology, 2022.